for small gap, digital nerve repair,
how often is primary repair really possible?
challenging the standard of suture-only primary repair
Direct repair, also commonly known as primary repair, is the most performed type of nerve repair. From 2018 to 2020, 63% and 57% of nerve repairs in U.S. inpatient and outpatient settings were coded as direct repair.1 As commonly as this type of repair is performed, outcomes are highly variable. In one study, 32% of patients undergoing surgery for painful neuroma had a failed direct repair.2
Tension-free primary repair is the ideal scenario, but how often is that really possible, especially when it comes to nerve repair in the hand? A recent survey of 150 hand fellowship–trained surgeons revealed that an average of 15% of their direct repairs separate and require a revision surgery.1
when it comes to nerve repair, technique is everything
From tension and adequate trimming to proper alignment and blood flow, there are many factors to consider when weighing the options of how best to repair a nerve injury.
Surgical repair techniques such as Connector-Assisted Repair® (CAR) or nerve grafts remove barriers to functional recovery, like tension, and increase the likelihood of long-term success and improved quality of life (QoL) for your patients.3
Tension is a combination of stress, strain and stretch, all of which can impact nerve regeneration. The challenge is that it’s difficult to observe the amount of tension a nerve is experiencing in a surgical scenario.
As little as 7-8% elongation or stretching of the nerve due to tension results in a 50% decrease in blood flow and an almost 30% reduction in axonal outgrowth.4,5
Minimizing tension is paramount to achieving optimal outcomes—especially at the most important zone of regeneration: the repair site. Normally, tension is distributed along the length of the nerve. Once that nerve is transected, the proper tension distribution cannot be restored as tension becomes concentrated at the repair site.
Connector-Assisted Repair alleviates tension by moving the suture-related strain away from the repair site, helping to minimize localized inflammation at the site of regeneration.6
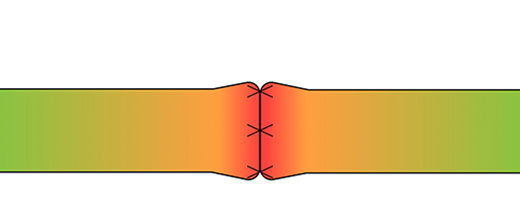
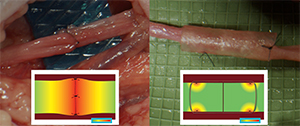
direct repair
Tension map highlighting the localized tensions at the coaptation site in direct repairs7
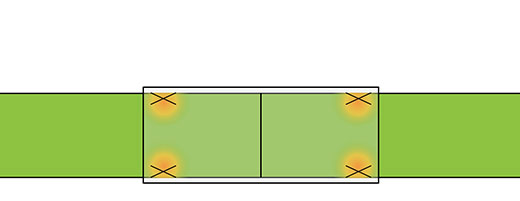
connector-assisted repair
Tension map highlighting tension concentrated away from the coaptation site with a Connector-Assisted Repair7
What happens when tension is present
When tension occurs, it can result in ischemia, reducing crucial intraneural blood supply.
Repair under tension can lead to misaligned fascicles, axonal escape and resultant neuroma formation.8 When tension is minimized through use of a connector, it reduces the risk of ischemia, and makes it easier to achieve better alignment of nerve ends, which reduces the risk of forced fascicular mismatch and neuroma formation.9
fascicular misalignment
Fascicular misalignment resulting from the over-tightening of suture.
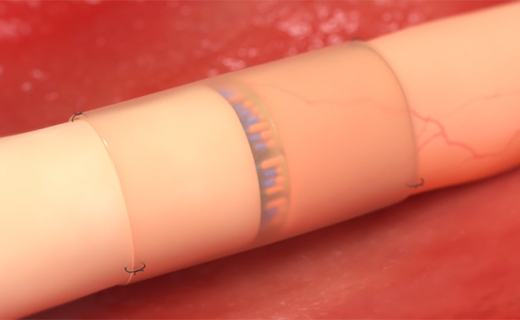
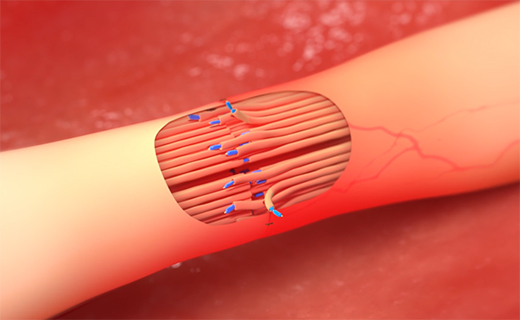
fascicular alignment
Fascicular alignment and appropriate axonal growth facilitated by a Connector-Assisted Repair.
When nerve repair techniques that offload tension at the coaptation site are used, rehabilitation protocols can shift to allow patients to begin mobility exercises sooner. And data shows that early mobilization is key,10 particularly in concomitant injuries of a nerve and tendon, which may occur up to 40% of the time in digital nerve injuries.11
In patients with acute limb injuries, early mobilization decreases pain and swelling, and improves functional outcomes compared with cast immobilization.11
failed direct repair
Neurorrhaphy that requires flexion limits range of motion, and if it is performed under tension the coaptation can fail, which leads to a need for secondary surgery.
the tension-free solution for your surgical expertise
mobility matters
Primary repair concentrates tension at the critical zone of regeneration. Connector-Assisted Repair reduces tension at this critical zone for nerve regeneration to allow for early range of motion and decreases the chance for primary repair failure.
Resecting the nerve back to healthy fascicles is essential to nerve regeneration. If you start with damaged fascicles, you end with damaged fascicles. Axons cannot properly regenerate through damaged tissue, so getting outside the zone of injury gives nerves a better chance of healthy recovery.
Certain factors may influence the decision to perform a primary repair, including:
- Mechanism of injury
- Nerve diameter
- Proximity to joint
- Joint immobilization
- Concomitant injuries (tendon or vascular injury)
- Post-operative therapy
Mechanism and zone of nerve injury
When a nerve is cut, the mechanism may have a significant impact on the integrity and roughness of the cut surface.
“Clean” cuts, like a glass or a knife injury, are sometimes considered to be ideal candidates for suture-only direct repair. However, even in these cases, the zone of injury extends beyond what is easily observable upon examination.
Research suggests that a nerve should be stabilized and transected with a thin sharp blade.12 It has been demonstrated that both sharp scissors and a no. 11 scalpel blade show significantly less surface area roughness compared to a razor blade, despite what may otherwise appear as a “clean” cut.13
These images show SEMs of nerves cut by a sharp piece of glass and fresh kitchen knife in comparison to nerve trimmed with a fresh surgical scalpel, demonstrating the impact that even the sharpest injury mechanisms can have to surrounding nerve tissue.1
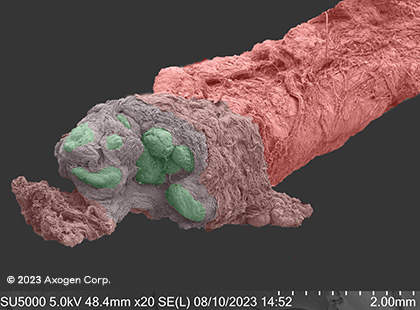
glass
Dry SEM
Ulnar nerve at wrist level
red: epinuerium | green: fascicles | yellow: connective tissue
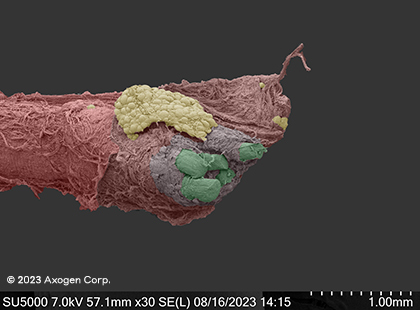
kitchen knife
Dry SEM
Common digital nerve
red: epinuerium | green: fascicles | yellow: connective tissue
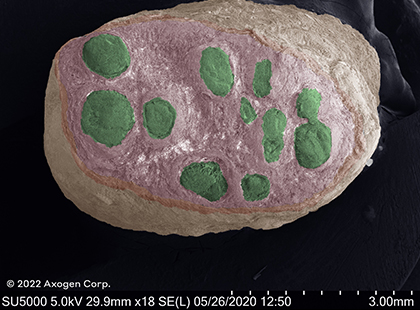
surgical cut
Cryo SEM
Common digital nerve
red: epinuerium | green: fascicles | yellow: connective tissue
Pre-clinical evidence shows that primary repair can diminish outcomes.
- Blood flow
- Axonal outgrowth
- elongation (%)
An elongation or stretching of the nerve due to tension by as little as 8% decreases blood flow by up to 50%.4,5
Mechanical failure occurs after elongation of 16% to 17%.14
- elongation
One study found that nerve repair under tension reduces axonal outgrowth, which can be associated to the status of Schwann cells in the distal nerve segment.5 As the nerves stretch due to tension, axonal outgrowth decreases.5 This makes it harder for axons to reach their intended targets and reestablish proper neural connectivity.
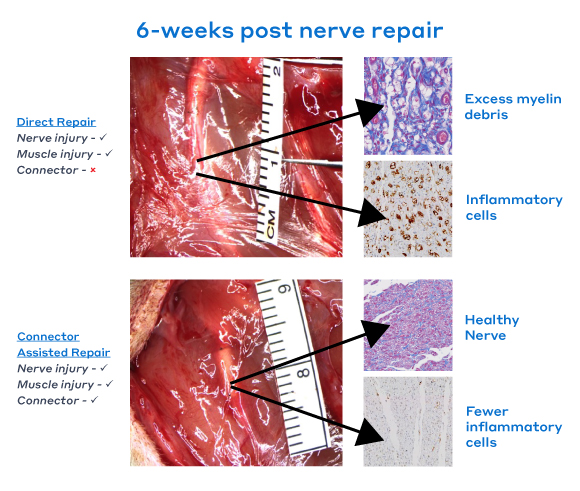
myelin debris
Six weeks after surrounding tissue injury and sciatic nerve transection and repair in a rat, the direct repair group showed significantly more myelin debris and inflammatory cells within the nerve compared to the Connector-Assisted Repair group. These findings demonstrate the potential benefits of Connector-Assisted Repair in protecting the nerve during the healing process, leading to improved nerve health and reduced inflammatory cells within the nerve.1
Patient follow-up after surgical intervention is challenging, especially for nerve-related injuries. Patients do not always reliably adhere to post-surgical rehabilitation plans, and compliance can be even more inconsistent in recovery from traumatic injuries due to the nature of how the injury occurred.
As a result, gathering and understanding a meaningful volume of data when it comes to outcomes of nerve repairs is not often possible for individual surgeons. Because of this, reinforcing a suture-only direct repair with a coaptation aid or protector can help to safe-guard potentially non-compliant patients from poor functional recovery or even failure.
percent of direct repairs that separate and require revision surgery (%)
Results based on a recent self-reported survey of 150 hand fellowship–trained surgeons1
Base: N=272 (2018 n=122, 2022 n=150)
^Letters indicate statistical significance at 95%
Connector-Assisted Repair and graft repairs enable easier technique and more consistent outcomes than suture-only direct repair.
See sizing and IFU on solution pages.

Nerve allografts are specifically designed to maintain both the natural nerve structure and biological activity of native nerve. They are a clinically proven, off-the-shelf solution with 82% meaningful recovery* in sensory, mixed and motor nerve gaps up to 70 mm.15


There is 50% increased likelihood of pain at the coaptation site when primary suture is used versus CAR with various conduits.4 Connector-Assisted Repair provides an alternative to direct repair that aids in alignment of nerve ends and reduces the potential for axonal escape and resultant painful neuroma formation.

![]()
Remodeling extracellular matrix for long-term protection with a short-term gel coating for enhanced nerve gliding and minimization of soft tissue attachments.
It’s important to use your algorithm, no matter the circumstances. We understand that when there are financial pressures involved, you may not want to add cost to a primary repair. There may be a common perception that allograft and Connector-Assisted Repair aren’t cost-efficient. Fortunately, there have been recent improvements in the reimbursement landscape.

Medicare outpatient facility payments for most direct nerve repair procedures decreased approximately 60% in 2020 and have sustained that through 2023.
connect with a nerve rep
There’s only a short form between you and our nerve product team who can help you get more information about our nerve repair solutions.
explore educational events
Axogen offers a robust variety of events and opportunities for you to interact with experts and stay up to date on the most recent happenings in peripheral nerve surgery. Learn more about and practice techniques related to Connector-Assisted Repair.
Sign up for our newsletter to get the latest research, news and in-depth insights about nerve repair.
references
- Axogen data on file.
- Jain SA, et al. Clinical outcomes of symptomatic neuroma resection and reconstruction with processed nerve allograft. Plast Reconstr Surg Glob Open. 2021;9(10):e3832. Published 2021 Oct 4. doi:10.1097/GOX.0000000000003832
- Ducic I, et al. Refinements of nerve repair with connector-assisted coaptation. 2017;37(3):256-263. doi:10.1002/micr.30151
- Babu P, et al. Entubulation techniques in peripheral nerve repair. Indian J Neurotrauma. 2008;5:15-20.
- Yi C, et al. Impaired nerve regeneration and Schwann cell activation after repair with tension. NeuroReport. 2010;21:958-962.
- Postlethwait RW, et al. Human tissue reaction to sutures. Ann Surg. 1975 Feb;181(2):144-50. doi:10.1097/00000658-197502000-00003
- Emily Jewell, MD. Nerve De-tensioning Effects of Conduits: A Quantitative Cadaveric Analysis Comparing Conduit-Assisted and Direct Digital Nerve Repairs. Paper presented at: AAHS 2023 Annual Meeting;January 17-21, 2023;Miami, FL. Accessed September, 28, 2023.
- Isaacs J, et al. Technical Assessment of Connector-Assisted Nerve Repair. J Hand Surg Am. 2016;41(7):760-766. doi:10.1016/j.jhsa.2016.04.015.
- Evans PJ, et al. Selective reinnervation: a comparison of recovery following microsuture and conduit nerve repair. Brain Res. 1991 Sep 20;559(2):315-21. doi:10.1016/0006-8993(91)90018-q
- Mohtadi N. Injured limbs recover better with early mobilization and functional bracing than with cast immobilization. J Bone Joint Surg Am. 2005;87(5):1167. doi:10.2106/JBJS.8705.ebo3
- Evertsson L, et al. Incidence, demographics and rehabilitation after digital nerve injury: A population-based study of 1004 adult patients in Sweden. PLoS One. 2023;18(4):e0283907. Published 2023 Apr 7. doi:10.1371/journal.pone.0283907
- Smetana, BW, et al. Improving Nerve End Preparation for Neurorrhaphy through Use of a Circumferentially Constraining Surgical Device. Date. 06/28/2022. Cited https://meeting.handsurgery.org/abstracts/2018/HS101.cgi.
- Rose RA, et al. The Cutting Edge: Surface Texture Analysis following Resection of Nerve Stumps Using Various Instruments. Plast Reconstr Surg Glob Open. 2021;9(5):e3566. doi:10.1097/gox.0000000000003566.
- Clark WL, et al. Nerve tension and blood flow in a rat model of immediate and delayed repairs. J Hand Surg Am. 1992 Jul;17(4):677-87. doi:10.1016/0363-5023(92)90316-h
- Safa B, et al. Peripheral nerve repair throughout the body with processed nerve allografts: Results from a large multicenter study. Microsurgery. Jul 2020;40(5):527-537. doi:10.1002/micr.30574